The human brain is an electric machine. For over a century, doctors have treated epilepsy as a short circuit in that machine. They prescribe drugs to dampen the sparks and calm the storm. But for millions of people, this approach fails.
About one-third of epilepsy patients are “drug-resistant.” They take the pills. The seizures continue anyway. This leaves scientists with a massive mystery. Why do the drugs fail so many people?
A team at Georgetown University may have found the answer. The problem might not be the electrical wires (neurons). It might be the maintenance crew. A groundbreaking new study reveals that zombie cells epilepsy triggers are hiding in the brain’s immune support system, known as “glia.”
By targeting these “undead” cells, the researchers did something incredible. They did not just stop the seizures. They prevented the disease from taking hold entirely.
What Did the Scientists Discover?
The research team looked at brain tissue from patients with Temporal Lobe Epilepsy (TLE). This is the most common form of epilepsy in adults. They noticed something strange about the support cells.
These cells were not dead. They were not alive and dividing either. They were stuck in a state called senescence. You can think of this as “Zombie Mode.”
These zombie cells were abundant. The epileptic brains had five times more of them than healthy brains 1 Khan, T., et al. (2025). Senescent Cell Clearance Ameliorates Temporal Lobe Epilepsy. Annals of Neurology. https://doi.org/10.1002/ana.78118. This was shocking because the control group was actually older than the epilepsy patients. Usually, old cells belong to old people. In this case, the disease itself was aging the brain.
The team tested a bold idea. They used a special class of drugs called “senolytics” to kill these zombie cells in mice. The results were powerful:
- Seizures Dropped: The mice had far fewer seizures.
- Total Protection: About 33% of the mice never developed epilepsy at all.
- Memory Returned: The treated mice regained their ability to learn and remember.
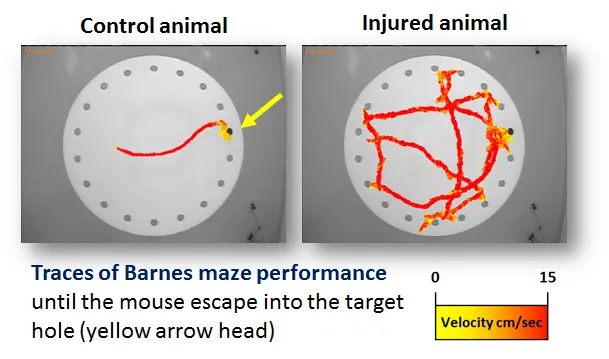
But an unexpecteded bonus result wasn’t just about seizures; it was about memory. To prove this, the scientists dropped the mice into a “Barnes Maze”—a bright, open table with 20 holes around the edge. Only one hole leads to a safe dark tunnel.
Untreated epileptic mice wandered aimlessly, unable to remember the escape route. But the mice treated with senolytics found the exit just as fast as healthy mice. This proved that clearing the zombie cells didn’t just stop the storm; it repaired the brain’s navigation system.
How Do Zombie Cells Harm the Brain?
To understand this discovery, you need to understand how a “zombie” cell works. It is not passive. It is destructive. We can explain this with The Rotten Apple Analogy.
Imagine your brain is a crate of fresh red apples. The apples represent your neurons. Now, imagine one apple begins to rot. This is the senescent cell.
A rotting apple releases ethylene gas. This gas touches the healthy apples nearby. It makes them ripen too fast and rot. Soon, the whole crate is spoiled.
Standard epilepsy drugs are like trying to polish the healthy apples. You might make them look nice for a moment. But you are ignoring the problem. The rotten apple is still there. It is still pumping out gas.
In the brain, this gas is a “toxic soup” of chemicals called the SASP 2 The Regeneration Center. (2025). Zombie Cells Explained: Senescence to Senolytic Therapy. The Regeneration Center. https://stemcellthailand.org/zombie-cells-senescence-senolytic-therapy/. This soup causes inflammation. It makes the nearby neurons hyper-active. This leads to seizures.
The Georgetown team used drugs to physically remove the rotten apple. Once the source of the toxicity was gone, the remaining apples (neurons) stayed healthy.
Who Are the Traitors in the Brain?
The study identified the specific type of cell that goes rogue. They are called microglia. Normally, these are the “gardeners” of the brain. They clean up waste and protect neurons.
But after a brain injury, these gardeners get overwhelmed. They stop cleaning. They switch into zombie mode. Instead of fixing the damage, they start spreading inflammation. This explains why a head injury today can turn into epilepsy months later.
Why Does This Change Everything?
This discovery offers a new hope called “Hit and Run” therapy. Current epilepsy drugs must be taken every day. If you miss a dose, you might have a seizure. They manage the symptoms forever.
Senolytics are different. You do not need to take them forever. The mice in the study were treated for only a few weeks. The drugs went in. They cleared the zombie cells. Then the treatment stopped.

Visualizing the Strategy: This conceptual illustration demonstrates the “Hit and Run” dosing model. Unlike daily pills, the drug is delivered in a short, intense “pulse” (Red), clearing the zombie cells and allowing for a long, drug-free recovery (Blue). Note: This is an artistic representation of the dosing schedule, not real patient data. Credit: Seriously Scientific.
The benefits lasted long after the drugs were gone. This suggests we could treat patients right after a brain injury to prevent epilepsy from ever starting. This is called anti-epileptogenesis 3 StatPearls. (2025). Mesial Temporal Lobe Epilepsy. NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK554432/.
What Are the Risks?
This is exciting, but we must be careful. The drugs used in the study included Dasatinib. This is a powerful chemotherapy drug used for leukemia 4 Open Exploration Publishing. (2025). FDA-approved kinase inhibitors: a promising therapeutic avenue for traumatic brain injury. Exploration of Neuroprotective Therapy. https://www.explorationpub.com/uploads/Article/A100877/100877.pdf. It has serious side effects. It can stress the heart and blood cells.
Also, inflammation is a double-edged sword. The brain needs some inflammation to heal after an injury. If we wipe out the microglia too soon, we might stop the healing process.
What Happens Next?
The path forward is clear. Scientists need to find the “Goldilocks” zone. They need to know exactly when to give the drugs and for how long. They also want to find safer drugs that target only the zombie cells without side effects.
Dr. Patrick Forcelli and his team are already looking toward clinical trials. If they succeed, we might finally have a cure that targets the root of the problem, not just the symptoms.


Author’s Note: What excites me most about this study isn’t just the seizure control, it’s the mechanism. 🧠
If clearing “zombie” glial cells can stop inflammation and rescue memory in epilepsy, where else could we apply this? This “Hit & Run” strategy opens some incredible doors:
Alzheimer’s & Dementia: Since these diseases are also driven by neuroinflammation and memory loss, could senolytics be the “brain reset” we’ve been looking for?
Concussions (TBI): Could a short course of these drugs immediately after a sports injury prevent the long-term brain damage (CTE) that athletes suffer from years later?
Stroke Recovery: Minimizing the “secondary damage” that happens after the initial stroke.
We are looking at a potential shift from “managing symptoms” to “clearing the damage.” Which application do you think researchers should prioritize next? 👇